Request for services:
- We can help your practice cash flow, reduce your cost & get paid faster.
- Medical Management Services is one of the leading Revenue Cycle management
- company. We provide end to end Revenue Cycle Management services to physicians,
- practices and hospitals.
- Our medical billing service is a hassle-free business solution for physicians, practices
- and hospital of any size. We offer a full range of practice management solutions to
- free you and your staff of tedious physician billing and remittance tasks. Helping you
- to focus on patient care and practice growth. We will work with you and your team
- to customize a solution that best suits the needs of your medical practice.
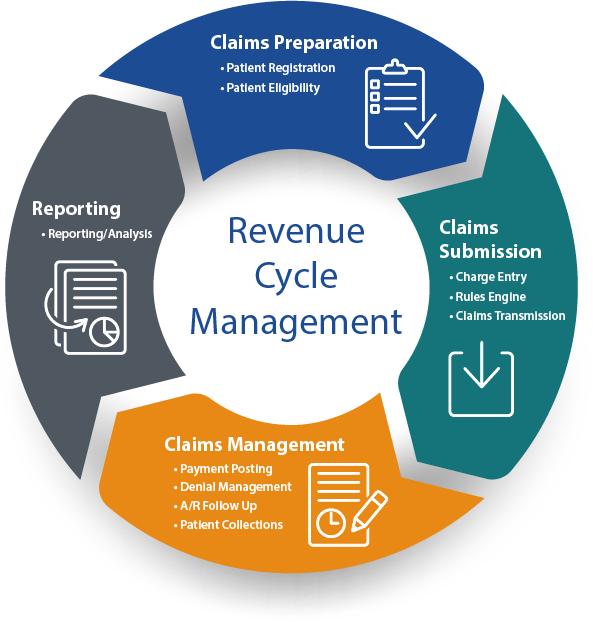
Complete medical billing service:
Our end-to-end medical billing services provide maximum reimbursement for our clients while reducing overall costs. We just don’t monitor your account we actively manage it.
Eligibility verification
Patient scheduling
Authorization request and tracking
ICD 10 – Medical coding
Charge entry
Electronic & paper claim submission
Payment posting
Denial review & management
Patient statements processing
Mailing/incoming patient calls
Old account receivables recovery
Extensive insurance follow-up
Custom practice management reports
Underpayment tracking
Credentialing or Enrollment
Provider Enrollment Services / Medical and Physician Credentialing Services
Rid yourself of all the headaches, mounds of paperwork, and confusion with the insurance companies!
Trust the experts at MMS Group to help you navigate the difficult process of provider enrollment and medical credentialing all at a low cost!
What you get with our Provider Enrollment and Physician Credentialing services:
An “All Purpose” credentialing manager to represent you with commercial and government payors.
We complete all applications and necessary paperwork on your behalf with the chosen payor networks and government entities.
Status reports so you know where you are in the process with each payor.
Maintain and update CAQH profile.
Complete all necessary credentialing requirements for each payor and follow through to completion.
Follow all payor contracts through to contract load date and provide copy of fully executed contract and fee schedules to your practice or billing company.
MMS Benefits:
Keep all your credentialing information in one place.
Years of experience to navigate through the process of Medicare and Medicaid provider enrollment, Commercial Insurance Provider Enrollment, and other healthcare provider credentialing needs.
Status reports keep you up to date on the progress of your credentialing
You and your medical office staff can focus on more important patient matters than dealing with enrollment paperwork
Joint Commission Credentialing Package (All Current Licenses, All Current DEA or CDS, Registration, NPDB, SAM, Board Certification if applicable, etc.)
Application collection services
Application completion
Data entry of paper applications
Ongoing monitoring services
Criminal background checks
Application mailing service
If you would like more information about, Billing, Medical Credentialing, free or paid membership, or other MMS services, please contact us at info@mmsgroup.us, call
Insurance Verification
Importance of Insurance Verification Services in Healthcare Industry
It is imperative that medical care providers understand the importance of insurance verification services in the healthcare industry. It plays a major role in a hospital’s claims denial management program. Successful billing depends on successful eligibility verification. Health insurance verification is all about the process of checking a patient’s active coverage with the insurance company and verifying the eligibility of his or her insurance claims.
In order to avoid claim rejection, the verification process must be done before the patient is admitted into a hospital. Otherwise, it might lead to denials and need for rework. Patients would be ineligible for benefits when they provide wrong or outdated information, or when their policies have been terminated or modified. A simple error can result in claim rejection or denial, so you have to be sure it is being done correctly.
Maximize Reimbursement and Minimize Denials
Our health insurance verification specialist work with patients, complete paperwork, and verify patient information with the insurance carrier to maximize reimbursement and facilitate revenue cycle improvement.
The service includes verification of:
Payable benefits
Co-pays
Co-insurances
Deductibles
Patient policy status
Effective date
Type of plan and coverage details
Plan exclusions
Claims mailing address
Referrals & pre-authorizations
Life time maximum, and more
Old AR Recovery
AR Recovery SERVICES
MMS Group offers a comprehensive range of healthcare recovery and AR management services to meet the unique needs of your organization. We employ accurate, aggressive, and effective tactics to optimize your medical account receivable collection ratio. And unlike most medical billing companies that only offer AR recovery solutions as part of a revenue cycle management package, MMS Group understands that no two healthcare facilities have the same needs.
We offer AR medical recovery services as a standalone option because we don’t believe in a one-size-fits-all approach to healthcare recovery solutions. Our dedicated team of AR recovery professionals focuses exclusively on investigating and resolving your old and ongoing AR accounts. And we’re experts at what we do. How do we do it? With a balanced four-part strategy.
